Introduction
The Pitt — Episode 3, Hank's assessment scene:
"Pulse 120. Pressure 100 over 65." — Nursing
"Small pericardial effusion, no evidence of tamponade yet." — Physician at ultrasound
"Watch the pressure. If it drops further, we operate right here." — Dr. Garcia
Although pulsus paradoxus is not explicitly named in this scene, it is implicit in the entire clinical reasoning guiding Hank's evaluation. Continuous blood pressure monitoring and attention to its variation during the respiratory cycle are part of the clinical examination that precedes and accompanies any suspicion of cardiac tamponade.
Pulsus paradoxus is one of the oldest and most elegant physical signs in clinical medicine — described more than 150 years ago by Kussmaul, still detectable at the bedside today without any special equipment other than a sphygmomanometer.
What is Pulsus Paradoxus?
Pulsus paradoxus is the exaggerated drop in systolic blood pressure during normal inspiration. Physiologically, systolic pressure drops slightly during inspiration — around 5 to 10 mmHg. When this drop exceeds 10 mmHg, pathological pulsus paradoxus is defined.
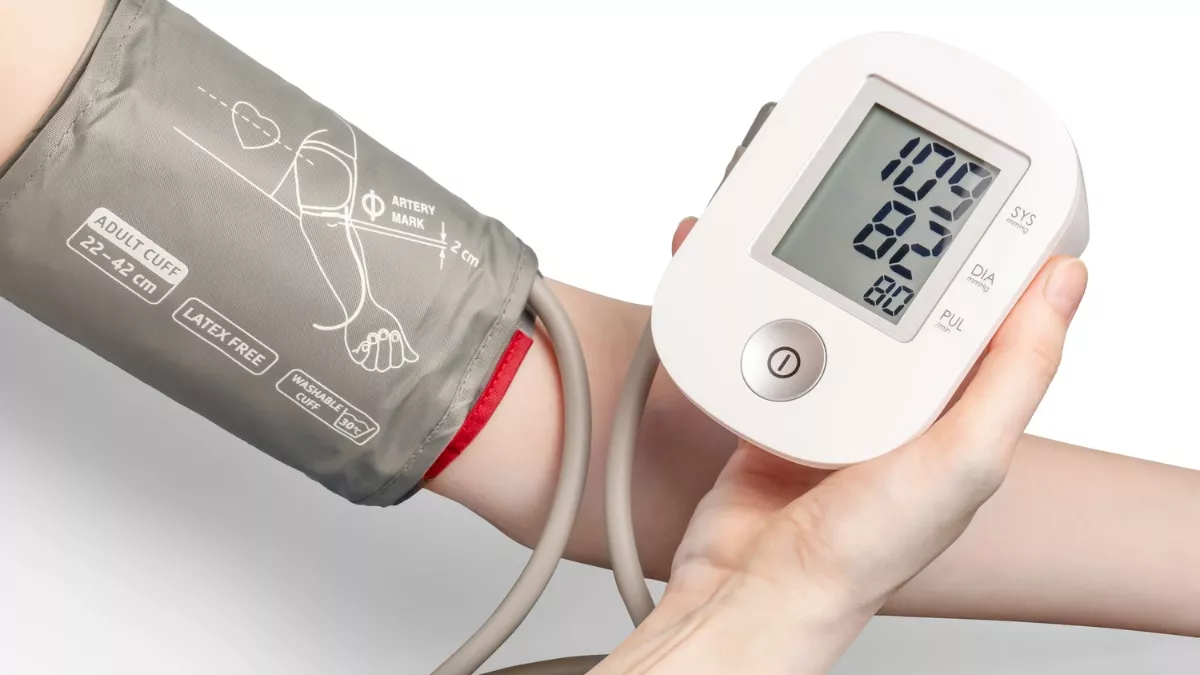
The name "paradoxical" comes from Kussmaul's historical observation in 1873: the heart continued beating — he could feel the pulse in the neck — but during inspiration the radial pulse completely disappeared. The heart was beating but the pulsation was not reaching the wrist. This seemed paradoxical.
The physiological mechanism is:
- During inspiration, intrathoracic pressure falls — which increases venous return to the right ventricle
- The distended RV pushes the interventricular septum to the left, reducing LV diastolic volume
- The LV pumps less blood with each inspiration — systolic pressure falls
- In cardiac tamponade, this mechanism is amplified by elevated intrapericardial pressure, which already limits filling of all chambers — any additional respiratory cycle variation amplifies the drop
Beyond tamponade, pulsus paradoxus occurs in other conditions that increase ventricular interdependence or negative intrathoracic pressure.
Causes and Clinical Context
The main causes of pulsus paradoxus include:
- Cardiac tamponade: most important cause in emergencies — pulsus paradoxus above 10 mmHg has 82% sensitivity and 75% specificity for tamponade
- Severe asthma or COPD exacerbation: generation of very negative intrathoracic pressure during respiratory effort amplifies ventricular interdependence
- Constrictive pericarditis: the fibrosed pericardium limits cardiac filling similarly to tamponade
- Massive pulmonary embolism: acute RV overload with septal shift
- Obstructive shock from other causes
In severe asthma — like the bronchospasm patient mentioned at the beginning of the episode — pulsus paradoxus can be as intense as in tamponade. That is why clinical context is fundamental for interpreting the sign.
Signs and Symptoms
Pulsus paradoxus itself is a physical sign — it does not cause symptoms. Symptoms come from the underlying condition:
In cardiac tamponade:
- Progressive dyspnea
- Hypotension
- Compensatory tachycardia
- Jugular venous distension
- Muffled heart sounds
In severe asthma:
- Intense dyspnea with wheezing
- Marked respiratory effort
- Accessory muscle use
- Falling SpO2
Intense pulsus paradoxus — above 20 mmHg — in an asthmatic patient is a severity sign indicating a severe attack with risk of respiratory failure.
Diagnosis
Pulsus paradoxus is measured with a sphygmomanometer and stethoscope:
- Inflate the cuff above the known systolic pressure
- Deflate slowly — 2 mmHg per second
- Identify the pressure at which Korotkoff sounds appear only during expiration
- Continue deflating until sounds appear during the entire respiratory cycle — both inspiration and expiration
- The difference between the two pressures is the pulsus paradoxus value
- Difference greater than 10 mmHg = pathological pulsus paradoxus
In mechanically ventilated patients, pulsus paradoxus is not assessable in the same way — mechanical ventilation reverses intrathoracic pressure gradients, and pulse pressure variation during the ventilatory cycle is used as an alternative fluid responsiveness index.
Emergency Treatment
Treatment of pulsus paradoxus is treatment of the underlying cause:
- Cardiac tamponade: ultrasound-guided percutaneous pericardiocentesis or emergency thoracotomy in traumatic cases
- Severe asthma: nebulized bronchodilators (albuterol), systemic corticosteroids, IV magnesium, and in the most severe cases, non-invasive mechanical ventilation or intubation
- Constrictive pericarditis: elective surgical pericardiectomy
Resolution of pulsus paradoxus after treatment — especially after pericardial drainage — is a clinical sign of immediate therapeutic success.
Prognosis and Complications
Pulsus paradoxus is a warning sign, not a complication in itself. Its severity reflects that of the underlying condition:
- In tamponade, pulsus paradoxus above 20 mmHg indicates severe hemodynamic compromise with immediate risk of cardiovascular collapse
- In asthma, pulsus paradoxus above 20–25 mmHg indicates a potentially fatal attack
- The absence of pulsus paradoxus in tamponade may indicate coexisting severe left ventricular dysfunction — which equalizes the bilateral pressure drop

Frequently Asked Questions
Why is it called paradoxical?
The name was given by Kussmaul in 1873 upon observing that, in certain patients with constrictive pericarditis, the heart continued beating normally (detectable by the jugular venous pulse) but the radial arterial pulse disappeared completely during inspiration — the heart was beating but the pulse was not felt, which seemed paradoxical. Today we know it is not a paradox, but a pathological exacerbation of a normal physiological variation.
Does everyone have some degree of pulsus paradoxus?
Yes. A 5 to 10 mmHg drop in systolic pressure during inspiration is physiological and normal in anyone. Pathological pulsus paradoxus is defined when this drop exceeds 10 mmHg. In people with very intense respiratory effort — such as athletes at maximum exercise — drops of up to 15 mmHg can be observed without underlying pathology.
Can pulsus paradoxus be detected without a sphygmomanometer?
Yes, but less precisely. Radial pulse palpation during breathing can reveal pulse disappearance during inspiration in cases of intense pulsus paradoxus — above 20 mmHg. In more subtle cases, only sphygmomanometer measurement allows precise quantification.
Does pulsus paradoxus occur in intubated patients?
In mechanical ventilation, physiology reverses: intrathoracic pressure increases during inspiration — unlike spontaneous breathing. Therefore, conventional pulsus paradoxus is not assessable in intubated patients. Instead, pulse pressure variation (PPV) or stroke volume variation (SVV) during the ventilatory cycle are used as dynamic fluid responsiveness indices.
Conclusion
Pulsus paradoxus is an elegant and powerful clinical sign — detectable with hands and a sphygmomanometer, capable of revealing cardiac tamponade, severe asthma, and constrictive pericarditis with simple bedside measurements. As indirectly demonstrated in Episode 3 of The Pitt, continuous blood pressure monitoring and its variation are a fundamental part of clinical reasoning in the critically ill patient.
Explore more in our Medical Terms category. Also read about cardiac tamponade, pericardiocentesis, severe asthma crisis, and point-of-care ultrasound.
Disclaimer: This content is for educational purposes only and does not substitute professional medical evaluation, diagnosis, or treatment. In case of emergency, call 911 immediately.


