Introduction
The Pitt — Episode 3, diagnosis scene:
"If the carbon dioxide levels come back way too high — above 60 — it means his brain stem is not telling him to breathe." — Dr. Robby
"The CO2 came back at 82. It definitely means Nick's brainstem is not firing to make him breathe." — Team
"Brain death is the same as death." — Dr. Robby
The clarity with which Dr. Robby communicates Nick Bradley's diagnosis — an 18-year-old in fentanyl overdose — is simultaneously necessary and painful. "Brain death is the same as death." That sentence summarizes decades of medical, legal, and philosophical debate in a single statement that the family needed to hear to move forward.
Brain death is one of the most misunderstood terms by the general public — and one of the most precise in medicine. Understanding what it means, what defines it, and what it implies is essential for anyone who might face this diagnosis in a family member.
What is Brain Death?
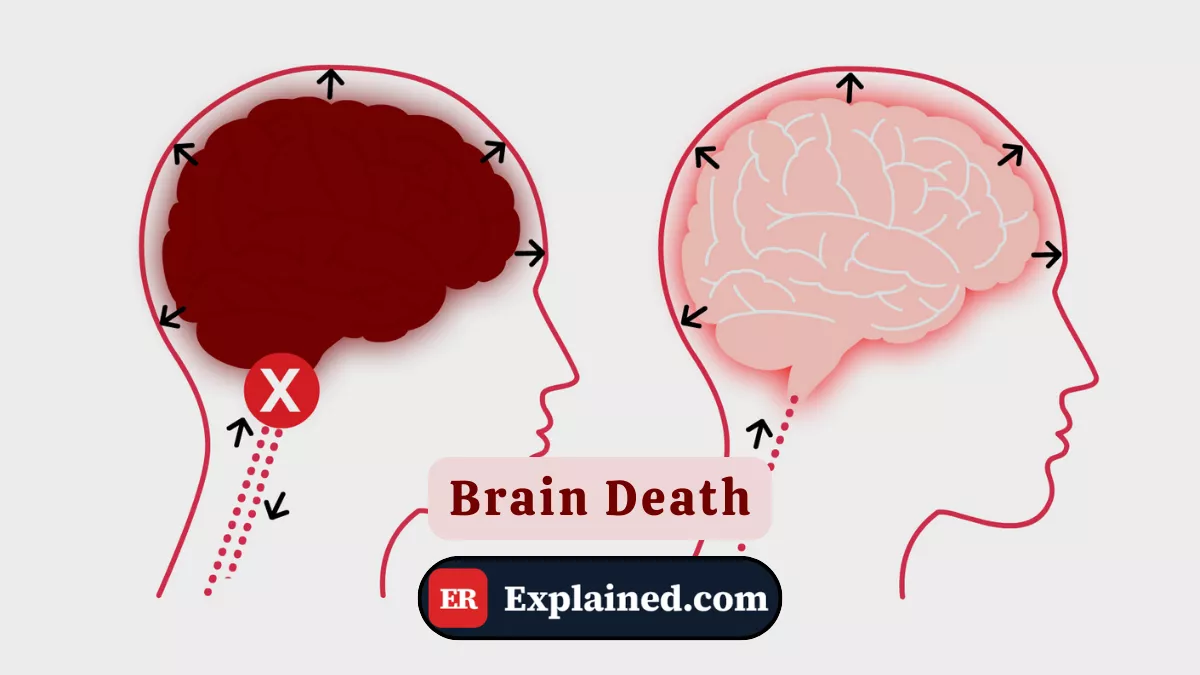
Brain death is the complete and irreversible cessation of all brain functions, including the cerebral cortex and the brainstem. It is legally equivalent to death in virtually all countries worldwide, including Brazil and the United States.

The definition requires three essential components:
- Irreversibility: cessation of brain functions is permanent and cannot be reversed by any available medical intervention
- Completeness: there is no residual brain function — neither cortical nor brainstem
- Known cause: the etiology of the coma is identified, documented, and sufficient to explain total brain destruction
It is essential to distinguish brain death from other altered consciousness states:
- Persistent vegetative state: absence of consciousness but with preserved brainstem functions — the patient breathes spontaneously
- Locked-in syndrome: preserved consciousness with near-total motor paralysis — the patient is awake and aware but cannot move
- Coma: deep depression of consciousness that is potentially reversible with treatment
In Nick's case, the fentanyl overdose caused cardiac arrest with prolonged time without cerebral perfusion — the global and prolonged hypoxia irreversibly destroyed the brain.
Causes and Clinical Context
The most common causes of brain death include:
- Global cerebral anoxia: cardiac arrest with delayed resuscitation — as in Nick's case — where prolonged hypoxia diffusely and irreversibly destroys the cerebral parenchyma
- Severe traumatic brain injury: with transtentorial cerebral herniation from intracranial hypertension
- Massive hemorrhagic stroke: devastating intraparenchymal or subarachnoid hemorrhage
- Ruptured cerebral aneurysm: subarachnoid hemorrhage with cerebral blood flow collapse
- Fulminant bacterial meningitis
The diagnosis is initiated when the patient is in deep coma with a known and irreversible cause, dependent on mechanical ventilation, and with no neurological response to stimuli.
Signs and Symptoms
The brain-dead patient presents a specific set of clinical findings, all derived from the absence of brainstem function:
- Deep coma: Glasgow 3 — no eye opening, no verbal response, no motor response to any stimulus
- Absent bilateral pupillary reflex: fixed and dilated pupils, no response to light
- Absent oculocephalic reflex: eyes do not move when the head is passively turned — absent "doll's eyes"
- Absent oculovestibular reflex: no ocular movement after cold water instillation in the ear canal
- Absent corneal reflex: no blinking when the cornea is touched
- Absent cough and gag reflexes
- Absent spontaneous breathing: confirmed by apnea test with PaCO2 above 60 mmHg without any respiratory movement — in Nick's case, CO2 reached 82 mmHg
Spinal reflex movements — such as limb flexion or extension to stimuli — may occur even in brain death, as the spinal cord may retain some reflex activity. These movements do not invalidate the diagnosis.
Diagnosis
Brain death diagnosis is rigorously protocolled. In the United States, determination requires:
Mandatory prerequisites:
- Identified, documented, and irreversible cause of coma
- Body temperature above 36°C
- Systolic blood pressure above 100 mmHg
- Absence of sedative effects, neuromuscular blockers, or severe metabolic disturbances
Clinical assessment: complete neurological examination — demonstrating absence of all brainstem reflexes — performed by qualified physicians per institutional protocol.
Apnea test: ventilator disconnection with oxygen delivery and CO2 monitoring for 10 minutes. Positive result: PaCO2 equal to or above 60 mmHg without any spontaneous breathing.
Confirmatory ancillary tests: when clinically indicated — EEG, transcranial Doppler, or cerebral perfusion scintigraphy. The scintigraphy performed for Nick showed the hollow skull sign — complete absence of intracranial uptake.
Emergency Treatment
After brain death confirmation, there is no treatment — the patient is dead. Subsequent management depends on context:
- Support maintenance for organ donation: when the family consents to donation, ventilatory and hemodynamic support is maintained to preserve organ viability until surgical procurement
- Ventilatory support withdrawal: terminal extubation with comfort care when there is no donation — as occurred with Nick after the family decision
- Family communication: a fundamental step requiring clarity, respect, and adequate time for family members to understand and process the diagnosis
Prognosis and Complications
Brain death is, by definition, irreversible. There is no documented recovery from brain death truly confirmed by rigorous protocol.
Associated challenges include:
- Family conflict and difficulty accepting — common and expected, as demonstrated in the episode
- Progressive hemodynamic instability even with support — the organism without central neurological control tends toward organic collapse over hours to days
- Ethical and legal issues related to organ donation and the duration of support maintenance
Frequently Asked Questions
Are brain death and coma the same thing?
No. Coma is a deep depression of consciousness that may be reversible with treatment — infections, metabolic disturbances, or drug effects can cause coma that reverses when the cause is treated. Brain death is the complete and irreversible cessation of all brain activity — it is not a state of unconsciousness, it is the total and permanent absence of any brain function.
Can a patient with brain death recover?
No. When the diagnosis is made correctly, following the rigorous protocol with all prerequisites met and concordant confirmatory tests, brain death is irreversible. Reported cases of "recovery" after brain death invariably involve incorrect diagnosis — protocol not followed, prerequisites not met, or reversible conditions not excluded.
Does the heart still beat in brain death?
Yes, as long as there is adequate ventilatory and hemodynamic support. The heart has its own automaticity — its intrinsic pacemaker (sinoatrial node) functions independently of the brain. Brain-dead patients can have a beating heart, maintained body temperature, and functioning circulation — as long as the ventilator provides the breaths that the brainstem no longer commands.
Who can diagnose brain death in the US?
In the United States, brain death determination must be performed by a licensed physician with expertise in the diagnosis and familiar with the clinical criteria. Most institutions require two separate examinations by two different physicians. Specific requirements vary by state and institution — many require or strongly recommend a neurologist or neurosurgeon to be involved in the determination.
Conclusion
Brain death is one of the most precise — and most humanly significant — diagnoses in medicine. As portrayed with depth in Episode 3 of The Pitt, communicating this diagnosis requires both technical rigor and compassion — and Dr. Robby's sentence, "brain death is the same as death," synthesizes decades of science into words a grieving family can understand.
Explore more in our Medical Terms category. Also read about the apnea test, cerebral perfusion scintigraphy, terminal extubation, and brain death in the ER.
Disclaimer: This content is for educational purposes only and does not substitute professional medical evaluation, diagnosis, or treatment. In case of emergency, call 911 immediately.