Introduction
The Pitt — Episode 3, thoracotomy scene:
"He's decompensating. Prep for thoracotomy." — Dr. Garcia
"Blade ten. Metz. Finochietto retractor." — Surgeon
"Opening the pericardium. We have a finger on the wound." — Surgical team
Hank arrived in the ER with a nail gun projectile lodged in his heart. Within minutes, his blood pressure began to drop and the pericardial effusion detected by ultrasound progressed to tamponade with ventricular collapse. There was no time for the operating room. The decision was made: open the chest right there, in the emergency department.
Emergency thoracotomy — also called resuscitative thoracotomy — is one of the most dramatic and technically demanding procedures in emergency medicine. Performed outside the conventional surgical environment, in patients on the verge of irreversible cardiovascular collapse, it represents the extreme limit of what can be done to save a life.
What is Emergency Thoracotomy?
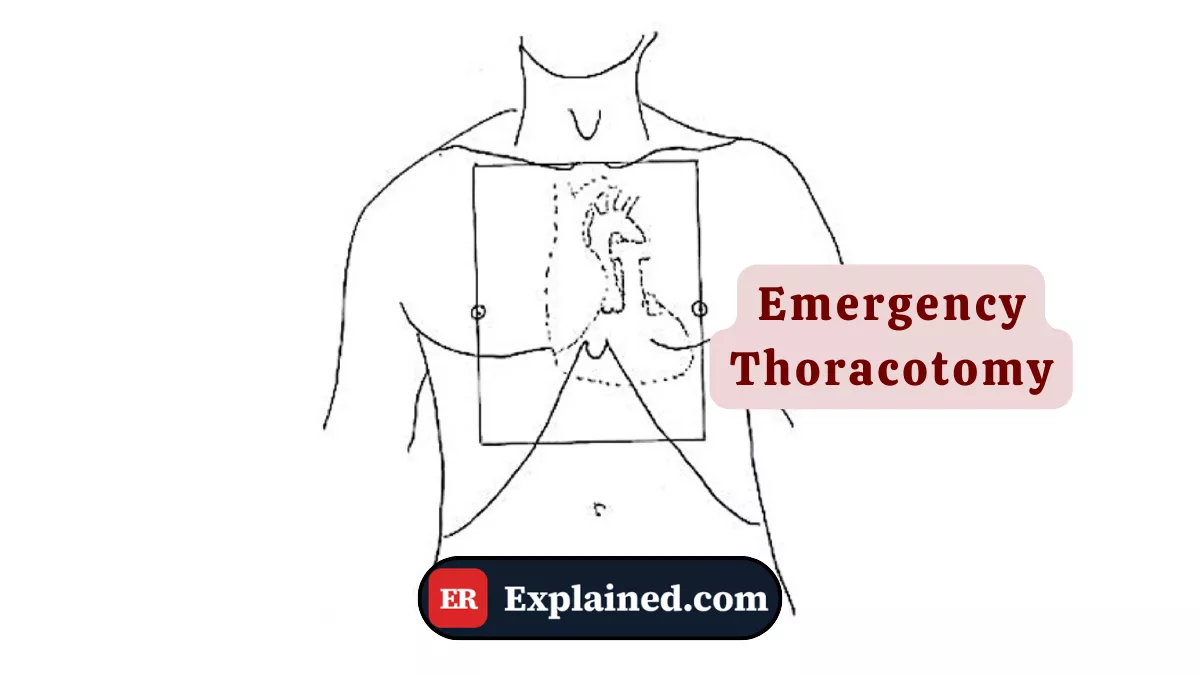
Emergency thoracotomy — or resuscitative thoracotomy — is the surgical opening of the thoracic cavity performed directly in the emergency department, without the full resources of a conventional operating room, in patients with imminent cardiovascular collapse or cardiac arrest caused by thoracic trauma.
The primary goal is to directly intervene on cardiac and vascular structures to:
- Relieve cardiac tamponade by decompressing the pericardium
- Control cardiac or great vessel hemorrhage through digital compression or direct suture
- Perform internal cardiac massage in refractory arrests
- Clamp the descending aorta to redistribute blood flow to the heart and brain
The most common approach is the left anterolateral thoracotomy — incision along the left fifth intercostal space — which provides rapid access to the heart, pericardium, and great vessels. The Finochietto retractor, as seen in the episode, is the instrument that keeps the intercostal space open throughout the procedure.
Causes and Clinical Context
Indications for emergency thoracotomy in the ER are restricted and well-defined by ACLS and Advanced Trauma Life Support (ATLS) guidelines:
- Penetrating thoracic trauma with recent signs of life: stab wounds, gunshot wounds, or penetrating objects — like the nail in the episode — with cardiovascular collapse occurring within the last 10 to 15 minutes.
- Cardiac tamponade refractory to pericardiocentesis: when percutaneous drainage is insufficient or technically unfeasible.
- Massive hemorrhage from intrathoracic great vessels.
- Massive pulmonary embolism with refractory cardiac arrest.
Emergency thoracotomy for blunt trauma — motor vehicle accidents, falls — has a far worse prognosis and is indicated more cautiously, as injuries are generally more extensive and diffuse.
The decision to perform the procedure in the ER rather than waiting for the operating room is made when transporting the patient would represent an imminent risk of death. In Hank's case, the progression of tamponade with ventricular collapse detected by ultrasound was the definitive trigger.
Signs and Symptoms
The patient who is a candidate for emergency thoracotomy presents an extremely critical picture:
- Severe hypotension refractory to fluids — systolic pressure below 60–70 mmHg
- Absent or progressively muffled heart sounds
- Neck vein distension — sign of tamponade or obstruction of venous return
- Progressive cyanosis and neurological deterioration
- Visible penetrating thoracic wound
- Cardiac arrest with pulseless electrical activity (PEA) of obstructive cause
On bedside ultrasound (eFAST), the decisive findings include pericardial effusion with diastolic collapse of the right ventricle — a direct sign of tamponade — and free fluid in the pleural space consistent with hemothorax.
Diagnosis
The indication for emergency thoracotomy is essentially clinical and sonographic:
eFAST: identifies pericardial effusion, hemothorax, and pneumothorax in under 2 minutes. In the episode, the sequential ultrasound exams revealed progression of the effusion to tamponade with right ventricular collapse.
Dynamic hemodynamic assessment: the response — or lack of response — to fluid resuscitation and vasoactive drugs defines the urgency of surgical intervention.
Trauma mechanism: the penetrating nature of the injury and its anatomical location guide the probability of involved cardiac or vascular structures.
There is no time for CT scanning or laboratory tests in patients with an indication for emergency thoracotomy. The decision must be made with available data in under 2 to 3 minutes.
The Procedure in the ER
The left anterolateral thoracotomy follows this technical sequence:
- Position the patient supine with the left arm abducted above the head.
- Perform rapid antisepsis of the left hemithorax with alcoholic chlorhexidine.
- Incise with a blade 10 scalpel along the left 5th intercostal space, from the parasternal line to the posterior axillary line.
- Deepen the incision through the intercostal muscles along the superior edge of the lower rib — to avoid the neurovascular bundle.
- Insert the Finochietto retractor blades and progressively open the intercostal space.
- Advance the endotracheal tube into the right main bronchus to isolate the left lung from the surgical field.
- Identify and open the pericardium longitudinally, anterior to the phrenic nerve, to access the heart.
- Apply digital compression over the ventricular wound for immediate hemorrhage control.
- Suture the cardiac injury with 2-0 Prolene in a horizontal mattress pattern over the compressing finger.
- Verify hemostasis, irrigate the cavity, and prepare for transfer to the operating room.
In the episode, after opening with the Finochietto retractor and the pericardium, the team identified a single perforation in the left ventricle from the nail. Control was achieved with immediate digital compression followed by suture — exactly the standard protocol for isolated penetrating cardiac wounds.
Prognosis and Complications
The prognosis of emergency thoracotomy varies widely with mechanism and time to intervention:
- Isolated penetrating cardiac wounds (such as Hank's case): survival of 60 to 70% when operated quickly by an experienced team.
- Gunshot wounds with multiple involved structures: survival of 15 to 30%.
- Blunt trauma with asystole: survival below 2%.
The main complications include:
- Surgical site infection and pleural empyema
- Phrenic nerve injury with diaphragmatic paralysis
- Post-operative cardiac arrhythmias
- Rib fractures from excessive retractor opening
- Lung injury from compression during opening
Frequently Asked Questions
What is the difference between emergency and elective thoracotomy?
Emergency thoracotomy — or resuscitative — is performed in the ER in seconds or minutes, without formal general anesthesia, with the patient in imminent collapse. Elective thoracotomy is performed in the operating room under full general anesthesia, with a complete team and surgical planning. Risks and conditions are entirely different, although the opening technique is similar.
Why is the incision made along the superior edge of the lower rib?
Each rib has a neurovascular bundle — artery, vein, and intercostal nerve — running along its inferior edge. Cutting along the superior edge of the rib below avoids injuring these structures, preventing difficult-to-control arterial bleeding and chronic neuropathic pain after surgery. It is one of the fundamental rules of thoracic surgery.
Can emergency thoracotomy be performed by any physician?
Ideally, it should be performed by a thoracic or trauma surgeon. However, in situations of absolute emergency where no specialist is available and the patient is in imminent collapse, trained emergency physicians can and should perform the procedure. Resuscitative thoracotomy training is part of emergency medicine and advanced trauma education.
What happens after emergency thoracotomy?
If the patient survives initial hemorrhage control in the ER, they are immediately transferred to the operating room for definitive repair under general anesthesia and controlled conditions. Post-operative follow-up includes ICU care, respiratory physiotherapy, multimodal analgesia, and monitoring for infectious and late hemorrhagic complications.
Conclusion
Emergency thoracotomy represents the extreme limit of emergency medicine — a brutal intervention under imperfect conditions, with the sole goal of keeping the patient alive long enough to reach the operating room. As shown with precision in Episode 3 of The Pitt, it demands rapid decision-making, flawless technique, and a perfectly synchronized team.
Explore more in our Medical Procedures category. Also read about the Finochietto retractor, cardiac tamponade, point-of-care ultrasound, and penetrating cardiac trauma.
Disclaimer: This content is for educational purposes only and does not substitute professional medical evaluation, diagnosis, or treatment. In case of emergency, call 911 immediately.