Introduction
The Pitt — Episode 3, ER scene:
"He needs to be cardioverted now. Systolic is already at 90." — Medical team
"75 of propofol, slow IV push. Sync cardioversion at 200 joules." — Dr. Robby
"Clear. [shock] Sinus rhythm. We got him." — Team
In this high-tension scene, a 35-year-old architect arrives in the ER with palpitations and atrial fibrillation at a dangerous rate. His dropping blood pressure and racing heart demand immediate action: synchronized electrical cardioversion. Within seconds, the heart is "reset" to a normal rhythm with a precisely timed shock.
This scene captures, with remarkable accuracy, the central role that defibrillators and cardioverters play in emergency medicine. These are devices that literally put the heart back on track — and understanding how they work can mean the difference between life and death.
What is a Defibrillator and Cardioverter?
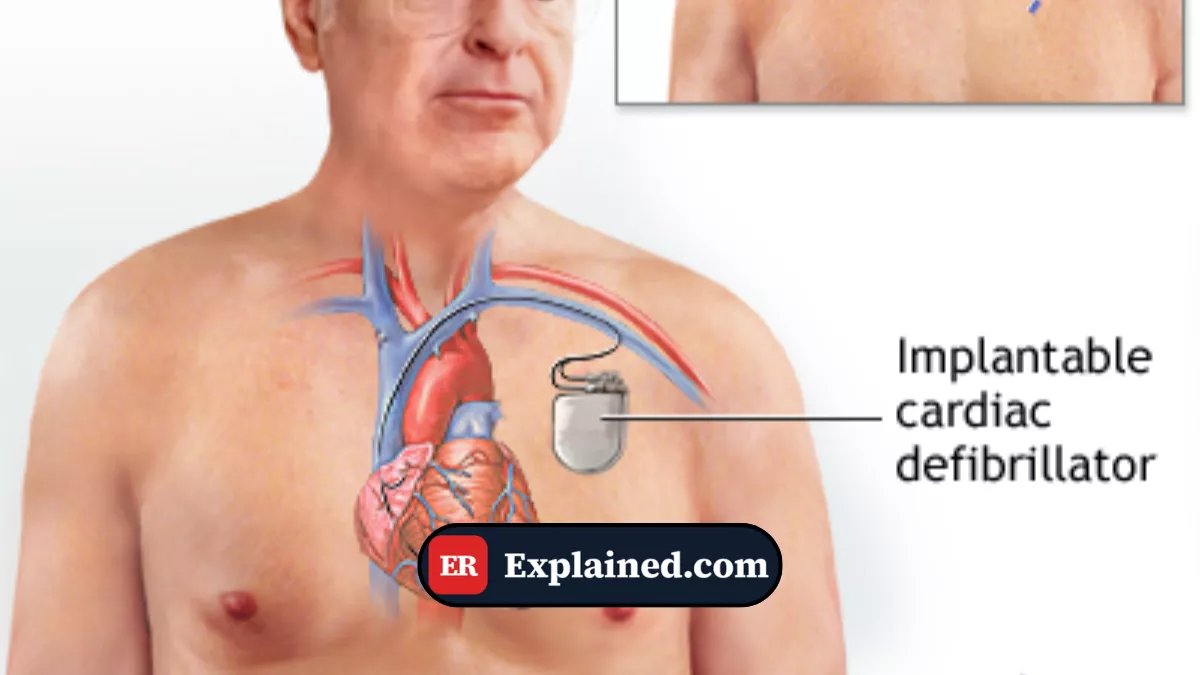
A defibrillator is a medical device that delivers a high-energy electrical current to the heart with the goal of terminating life-threatening arrhythmias, such as ventricular fibrillation (VF) and pulseless ventricular tachycardia (pVT). When the heart enters one of these rhythms, it loses the ability to pump blood effectively — and the electrical shock essentially "resets" the chaotic electrical activity, allowing the heart's natural pacemaker to regain control.

A cardioverter works in a similar fashion, but with one critical distinction: the shock is synchronized with the cardiac cycle — specifically timed to coincide with the R wave on the electrocardiogram. This prevents the discharge from falling during a vulnerable period of the cycle, which could trigger ventricular fibrillation. Synchronized cardioversion is used for arrhythmias with a present pulse, such as unstable atrial fibrillation (AFib), atrial flutter, and supraventricular tachycardia (SVT).
In modern hospital settings, both functions are typically integrated into a single multipurpose monitor-defibrillator unit. These devices are also capable of:
- Continuous cardiac rhythm monitoring
- 12-lead ECG acquisition and interpretation
- External transcutaneous pacing
- Pulse oximetry and capnography
In pre-hospital environments, the Automated External Defibrillator (AED) is designed for use by trained laypersons. It automatically analyzes the cardiac rhythm and guides the operator with voice commands, indicating whether a shock is advised.
Causes and Clinical Context
The use of a defibrillator or cardioverter is indicated whenever the heart presents such disorganized electrical activity that it severely compromises cardiac output. The main conditions that lead to the use of these devices include:
- Ventricular fibrillation (VF): the most common arrhythmia in sudden cardiac arrest, associated with coronary artery disease, acute myocardial infarction, and cardiomyopathies.
- Pulseless ventricular tachycardia (pVT): an organized rhythm on the monitor but with no effective perfusion. Requires immediate unsynchronized defibrillation.
- Unstable atrial fibrillation (AFib): as depicted in the episode, patients with recent-onset AFib (under 48 hours) and signs of hemodynamic instability — hypotension, chest pain, altered consciousness — are candidates for synchronized electrical cardioversion.
- Atrial flutter: typically requires lower energy for conversion, usually between 50 and 100 joules.
- Refractory supraventricular tachycardia (SVT): when vagal maneuvers and medications have failed.
Common precipitating factors include myocardial ischemia, electrolyte imbalances (hypokalemia, hypomagnesemia), drug or medication toxicity, severe hypoxia, and pre-existing structural heart disease. In the episode, the trigger was excessive nicotine use from vaping — the equivalent of two packs of cigarettes in a single night.
Signs and Symptoms
Early recognition of arrhythmias that require defibrillation or cardioversion is essential. Signs and symptoms vary depending on the type and severity of the arrhythmia:
In unstable arrhythmias with a pulse (cardioversion candidates):
- Rapid and irregular palpitations
- Hypotension (systolic blood pressure below 90 mmHg)
- Chest pain or discomfort
- Dyspnea and shortness of breath
- Dizziness, pre-syncope, or syncope
- Altered level of consciousness
In cardiac arrest (immediate defibrillation indicated):
- Absence of central pulse
- Sudden loss of consciousness
- Apnea or agonal breathing (gasping)
- Cyanosis of the lips and extremities
On the cardiac monitor, ventricular fibrillation appears as a completely chaotic and irregular line, while atrial fibrillation shows absence of defined P waves with an irregularly irregular ventricular response. Rapid rhythm recognition on the monitor is the trigger for immediate action.
Diagnosis
The diagnosis that indicates the use of a defibrillator or cardioverter is primarily clinical and electrocardiographic. The key steps include:
Primary assessment (ABCDE approach): assessing airway, breathing, circulation, disability, and exposure. In the absence of a pulse with a shockable rhythm on the monitor, defibrillation must occur within 2 minutes.
12-lead ECG: essential for identifying the arrhythmia type, the presence of blocks, signs of ischemia, and QT interval. In the episode, the patient's smartwatch was interrogated by the team to determine how long the AFib had been present — a critical data point for safe cardioversion.
Hemodynamic stability assessment: blood pressure, heart rate, level of consciousness, and signs of peripheral perfusion determine the urgency of the intervention.
Supplementary workup: serum electrolytes, renal function, complete blood count, and point-of-care echocardiography to assess ventricular function and rule out intracardiac thrombus.
Emergency Use
The protocol varies depending on the clinical situation. Here are the main approaches:
Defibrillation (unsynchronized) — Cardiac Arrest
- Confirm absence of pulse and shockable rhythm (VF or pVT) on the monitor.
- Begin high-quality CPR immediately.
- Position the pads: one below the right clavicle and one at the left midaxillary line.
- Charge the device to 200 joules (biphasic) or 360 joules (monophasic).
- Ensure all personnel are clear — announce loudly: "Clear!"
- Deliver the shock and immediately resume CPR.
- Reassess rhythm after 2 minutes of CPR.
Synchronized Cardioversion — Unstable Arrhythmia with Pulse
- Confirm indication: AFib, atrial flutter, SVT, or VT with pulse and hemodynamic instability.
- Sedate the patient with a fast-acting agent — in the episode, 75 mg of propofol slow IV push was used.
- Activate SYNC mode on the monitor-defibrillator to synchronize the shock with the R wave.
- Select energy: 100–200 joules for AFib; 50–100 joules for atrial flutter.
- Confirm all personnel are clear and deliver the shock.
- Immediately check the post-shock rhythm on the monitor.
- Repeat if necessary, escalating energy progressively.
After conversion, the patient should be monitored for several hours and the underlying cause of the arrhythmia should be investigated and addressed. In the episode, the team also referred the patient to addiction services — demonstrating that care extends well beyond the immediate shock.
Prognosis and Complications
When correctly performed within the appropriate therapeutic window, electrical cardioversion achieves a success rate exceeding 90% for restoring sinus rhythm in recent-onset AFib. In ventricular fibrillation, each minute without defibrillation reduces survival chances by 7% to 10%.
Possible complications include:
- Systemic embolism or ischemic stroke: increased risk in AFib lasting more than 48 hours, when a thrombus may have formed in the left atrium. This is exactly why the 12-hour safe window was emphasized in the episode.
- Post-cardioversion arrhythmias: transient bradycardia, premature beats, or rarely, VF induced by an unsynchronized shock.
- Mild skin burns at the pad contact sites.
- Post-cardioversion hypotension related to the sedative agent used.
Long-term prognosis depends on treating the underlying cause and adherence to outpatient cardiology follow-up.

Frequently Asked Questions
What is the difference between defibrillation and cardioversion?
Defibrillation is a high-energy, unsynchronized electrical shock used in cardiac arrest for ventricular fibrillation or pulseless ventricular tachycardia. Cardioversion is a synchronized shock timed to the R wave on the ECG, used for arrhythmias with a present but unstable pulse, such as atrial fibrillation. Synchronization prevents the shock from landing during a vulnerable phase of the cardiac cycle, which could otherwise induce ventricular fibrillation.
Does the patient need to be sedated for cardioversion?
Yes. In conscious patients, electrical cardioversion is a painful procedure. Sedation with a fast-acting agent is mandatory — options include propofol, midazolam, or etomidate. In the episode, 75 mg of propofol administered as a slow IV push was used. Continuous monitoring of oxygen saturation, blood pressure, and airway patency is required throughout the procedure.
Can anyone use an AED?
Yes. The Automated External Defibrillator (AED) was specifically designed for that purpose. It automatically analyzes the cardiac rhythm and provides voice instructions, indicating whether a shock is advised. In the U.S., many public spaces are required to have AEDs on-site. Any person trained in basic life support can — and should — use one in the event of a cardiac arrest. Time to first shock is the single most important factor in survival.
How many joules are used for atrial fibrillation cardioversion?
For atrial fibrillation, the initial recommended energy per ACLS (Advanced Cardiovascular Life Support) guidelines is 120 to 200 joules for biphasic devices. For atrial flutter, one may start with 50 to 100 joules. If the first shock is ineffective, energy is escalated progressively. Older monophasic devices typically use higher energies, ranging from 200 to 360 joules.
Conclusion
The defibrillator and cardioverter are among the most critical instruments in any emergency department. As shown in Episode 3 of The Pitt, the rapid identification of an unstable arrhythmia, proper sedation, and precise delivery of a synchronized shock were enough to restore sinus rhythm in a patient whose life was on the line — within minutes.
Understanding how these devices work — and when to use them — is essential for both healthcare professionals and laypeople who want to be prepared for a cardiac emergency.
Explore more related content on our site: learn about atrial fibrillation in the ER, the electrical cardioversion procedure, sedatives used in emergency medicine, and cardiac arrest management. Browse our full Medical Instruments category for more.
Disclaimer: This content is for educational purposes only and does not substitute professional medical evaluation, diagnosis, or treatment. In case of emergency, call 911 immediately.