Introduction
The Pitt — Episode 3, patient in shock scene:
"We can place a long catheter in his jugular vein, down into his heart, and administer Levophed to constrict his arteries and raise his blood pressure." — Dr. Robby
"But that could cause organ damage, organ failure." — Patient's family
"Each new step is even more invasive and could cause more suffering with minimal benefit." — Dr. Robby
This scene precisely captures the clinical dilemma surrounding central venous catheters in the ER: a powerful instrument capable of saving lives by providing deep vascular access for vasoactive drugs — but one that also carries risks and forces difficult decisions about how far to push life support.
The central venous catheter is one of the most versatile and essential devices in critical care and emergency medicine. Understanding when and how it is used helps healthcare professionals, patients, and families better grasp the decisions made in the most critical moments.
What is a Central Venous Catheter?
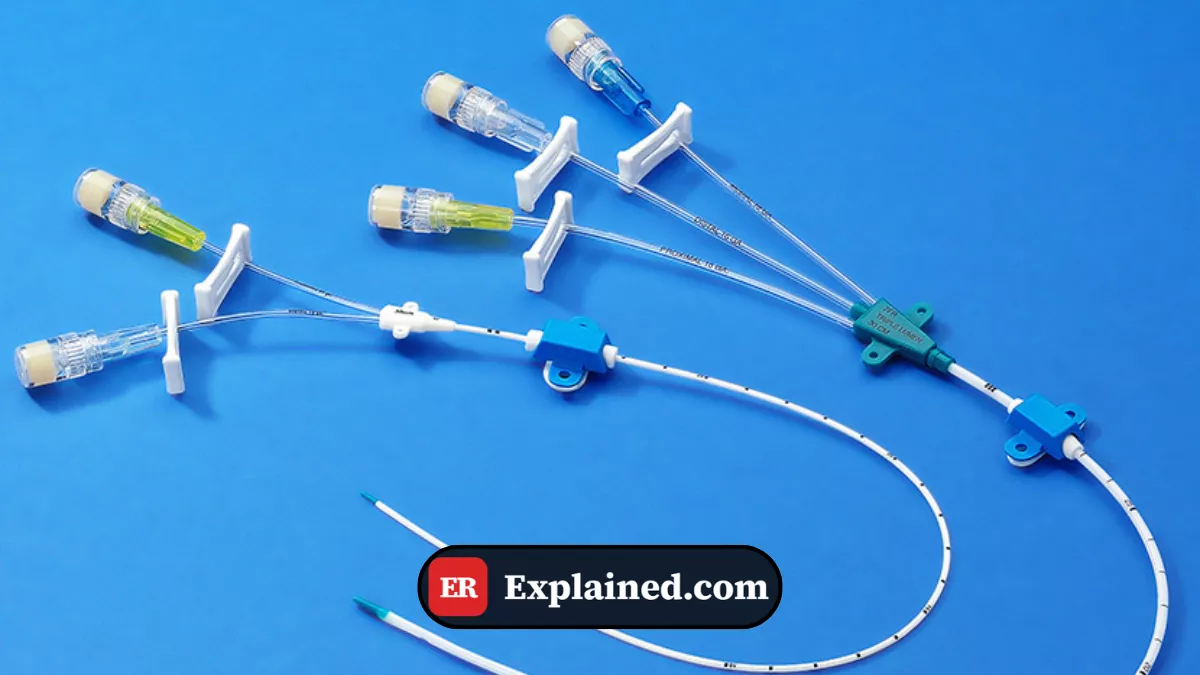
A central venous catheter (CVC) — also called a central line or deep venous access — is a flexible tubular device, usually made of polyurethane or silicone, inserted into a large-caliber vein that empties directly into the right cardiac chambers or the great thoracic veins.

The main access routes include:
- Internal jugular vein: lateral to the neck, between the sternocleidomastoid muscle. This is the preferred route in emergencies due to easy access and real-time ultrasound guidance.
- Subclavian vein: below the clavicle. Lower infection risk but higher risk of pneumothorax during insertion.
- Femoral vein: in the groin. Fast and safe access, but higher risk of thrombosis and infection with prolonged use.
The catheter may have a single lumen or multiple lumens, allowing simultaneous administration of several incompatible medications. Special models include the Swan-Ganz catheter for advanced hemodynamic monitoring and the dialysis catheter for renal replacement therapy.
Causes and Clinical Context
Central venous catheters are indicated in several emergency and critical care situations:
- Refractory shock: when the patient does not respond to peripheral IV fluids and requires vasoactive drugs such as norepinephrine (Levophed), dopamine, or vasopressin — which must not be administered through peripheral veins due to the risk of tissue necrosis.
- Lack of peripheral venous access: patients with collapsed veins due to severe shock, obesity, chronic IV drug use, or extensive burns.
- Central venous pressure (CVP) monitoring: to guide fluid resuscitation in critically ill patients.
- Total parenteral nutrition: hypertonic solutions that would damage peripheral veins.
- Urgent hemodialysis: in acute renal failure requiring renal replacement therapy.
- Chemotherapy administration and vesicant medications.
In the episode, the indication was distributive shock in the overdose patient — falling blood pressure, need for a potent vasopressor, and lack of response to fluids made central access indispensable.
Signs and Symptoms
The clinical situations that indicate central venous catheter use have recognizable features:
In shock:
- Persistent hypotension (systolic pressure below 90 mmHg)
- Compensatory tachycardia
- Cold, clammy extremities with prolonged capillary refill time
- Oliguria or anuria
- Altered level of consciousness
In peripheral access failure:
- No visible or palpable veins
- Multiple failed peripheral puncture attempts
- Urgent need for reliable vascular access
Early identification of these situations is crucial so that the indication for central access is made at the right time — neither too late, when the patient is already in total collapse, nor prematurely without adequate indication.
Diagnosis
The decision to insert a central venous catheter is based on integrated clinical assessment with complementary tests:
Hemodynamic assessment: invasive or non-invasive blood pressure, heart rate, urine output, and level of consciousness guide the urgency of central access.
Bedside ultrasound: essential for guiding catheter insertion in real time, reducing complications such as pneumothorax and accidental arterial puncture. Routine ultrasound use has reduced mechanical complication rates by up to 71% in published studies.
Arterial blood gas: assesses tissue perfusion, lactate levels, and need for advanced hemodynamic support.
Post-insertion chest X-ray: mandatory to confirm correct catheter tip position and rule out pneumothorax.
Emergency Use
Central venous catheter insertion follows a strict asepsis and technique protocol:
- Position the patient in Trendelenburg (head down) to distend the jugular vein and reduce the risk of air embolism.
- Perform broad antisepsis with alcoholic chlorhexidine and cover the field with sterile drapes.
- Identify the target vein with real-time ultrasound.
- Anesthetize the skin and subcutaneous tissue with 1% lidocaine.
- Puncture the vein with a large-bore needle, confirming reflux of dark venous blood.
- Introduce the metal guidewire (Seldinger technique) through the needle with gentle movements.
- Remove the needle while keeping the guidewire in place.
- Dilate the tract with the plastic dilator over the guidewire.
- Introduce the catheter over the guidewire to the appropriate depth — typically 15 cm on the right and 17 cm on the left via the internal jugular.
- Remove the guidewire, verify reflux in all lumens, and secure the catheter to the skin with suture.
- Apply a sterile occlusive dressing and request a confirmatory chest X-ray.
After radiological confirmation of position, the catheter is ready for use. In the episode, the goal was to administer norepinephrine (Levophed) — a potent vasopressor that must be infused exclusively through central access to avoid peripheral tissue necrosis.
Prognosis and Complications
When correctly inserted with adequate indication, the central venous catheter is a safe and highly effective instrument. However, its potential complications must be recognized:
- Pneumothorax: accidental lung puncture during subclavian access, with an incidence of 1 to 3%.
- Accidental arterial puncture: can cause an expanding cervical hematoma or hemothorax.
- Catheter-related bloodstream infection (CRBSI): the main complication with prolonged use, associated with high ICU mortality.
- Deep vein thrombosis: especially with femoral access.
- Air embolism: air entry through the lumen during insertion or catheter exchange.
- Cardiac arrhythmias from incorrect positioning of the catheter tip inside the heart.
The risk of complications is reduced with ultrasound use, strict aseptic technique, adequate team training, and early removal of the catheter when no longer necessary.

Frequently Asked Questions
What is the difference between a central venous catheter and peripheral IV access?
Peripheral IV access is inserted into superficial veins of the limbs — usually the forearm or dorsum of the hand — and is adequate for most hospital medications. A central venous catheter reaches large-caliber veins close to the heart and is required for vasoactive drugs, parenteral nutrition, CVP monitoring, and situations where peripheral access is not feasible or sufficient.
Is central venous catheter insertion painful?
The procedure is performed under local anesthesia with lidocaine, making insertion comfortable in most cases. Conscious patients may feel pressure or discomfort during tract dilation, but intense pain is not expected. In sedated patients or during cardiac arrest, the procedure is performed without additional anesthesia.
How long can the catheter remain in place?
There is no fixed deadline established, but guidelines recommend removing the catheter as soon as it is no longer needed to reduce infection risk. Jugular and subclavian catheters have lower infection risk than femoral ones. Dressing changes should be performed every 48 to 72 hours with strict aseptic technique.
What is the Seldinger technique?
The Seldinger technique is the standard method for vascular catheter insertion. It involves puncturing the vein with a thin needle, introducing a flexible metal guidewire through the needle, removing the needle while keeping the wire in place, dilating the tract, and finally sliding the catheter over the guidewire to the desired position. This technique minimizes vascular trauma and is widely used in central venous access, chest drainage, and other interventional procedures.
Conclusion
The central venous catheter is an indispensable instrument in emergency and critical care medicine. As depicted in Episode 3 of The Pitt, its indication involves not only technical skill but also a profound ethical reflection on the limits of life support — and what is truly best for the patient in that moment.
Explore more about emergency instruments and procedures in our Medical Instruments category. Also check out our articles on norepinephrine in the ER, septic shock, point-of-care ultrasound, and mechanical ventilator.
Disclaimer: This content is for educational purposes only and does not substitute professional medical evaluation, diagnosis, or treatment. In case of emergency, call 911 immediately.