The Threshold of Life
"For the apnea test, we keep him on 100% oxygen, but the ventilator won't be giving him breaths. For 10 minutes. If his carbon dioxide levels come back way too high, then we'll know that his brain stem is not telling him to breathe." — Emergency Room
One of the most difficult and emotionally devastating scenarios in emergency medicine and intensive care is the diagnosis of brain death. This frequently occurs after severe head trauma, a massive hemorrhagic stroke, or, tragically common, an anoxic brain injury caused by a drug overdose where the patient stopped breathing for too long.
The patient is warm to the touch. Their chest rises and falls. Their heart is beating on the monitor. To the family, it looks like the patient is just sleeping deeply.
But medically and legally, if the brain has irreversibly ceased all functions, the person is dead. The machines are merely ventilating a lifeless body.
What is Brain Death?
Brain death is not the same as a coma or a persistent vegetative state.

In a coma, the brain is damaged, but the basic vital functions controlled by the brainstem (like breathing and regulating heart rate) still work. The patient can potentially wake up.
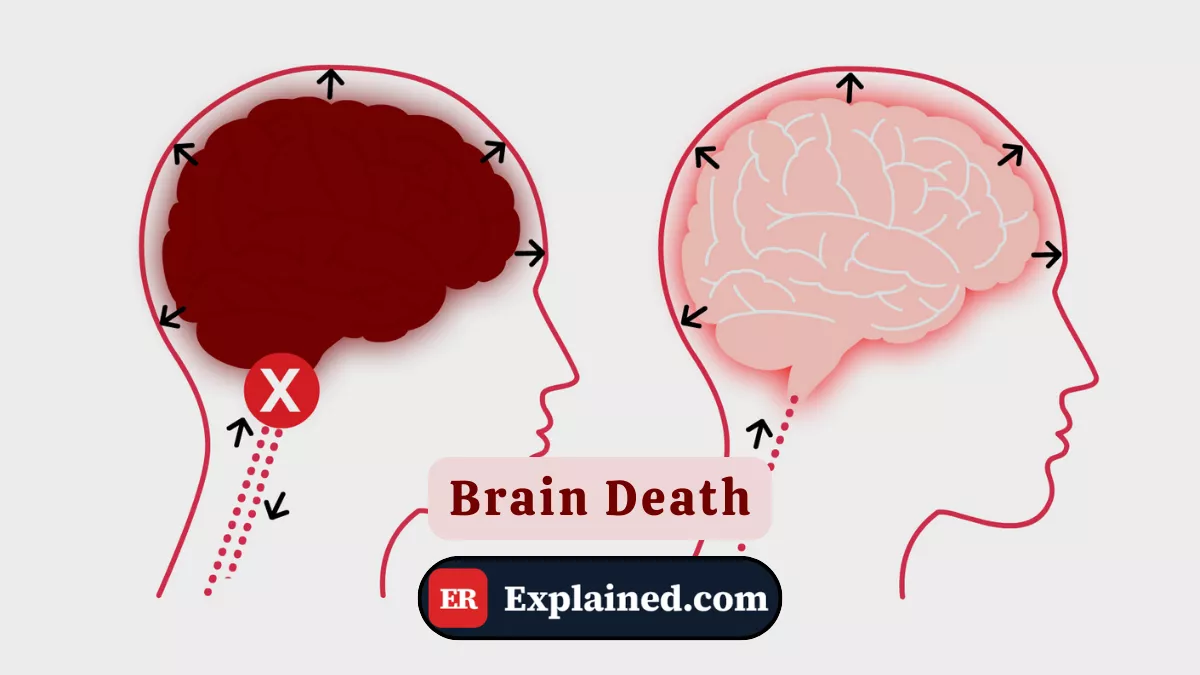
In brain death, the entire brain, including the cortex (responsible for thought) and the brainstem (responsible for basic survival), has been permanently destroyed, usually by extreme swelling that cut off all blood flow inside the skull.
The Clinical Neurological Exams
Before declaring brain death, doctors must perform a rigorous series of bedside clinical tests to prove the total absence of brainstem reflexes.
These tests include:
- Pupillary Reflex: Shining a bright light into the eyes. In a dead brain, the pupils remain fixed and dilated.
- Corneal Reflex: Touching the surface of the eye with a cotton swab. There will be no blinking.
- Oculocephalic Reflex (Doll's Eyes): Turning the head rapidly from side to side. The eyes move with the head instead of remaining fixed.
- Gag Reflex: Stimulating the back of the throat with a suction tube. There will be no coughing or gagging.
If the patient fails all these reflexes, the doctor proceeds to the final, definitive test.
The Apnea Test: The Definitive Proof
The Apnea Test is the gold standard for confirming brain death. It tests the most basic, primitive function of the human brain: the drive to breathe.
The procedure is executed with extreme caution:
- Pre-oxygenation: The patient is given 100% oxygen through the ventilator for several minutes to saturate their blood.
- Disconnection: The ventilator is paused. The machine stops pushing air into the lungs. Oxygen continues to flow passively through a tube, but no mechanical breaths are given.
- Observation (10 Minutes): The doctor watches the patient's chest. They are looking for any spontaneous attempt to breathe, even a tiny gasp.
- CO2 Buildup: Without the ventilator, carbon dioxide (CO2) builds up rapidly in the blood. In a living brain, high CO2 levels are the most powerful chemical trigger to force the body to take a breath.
- The Blood Test: After 10 minutes, arterial blood is drawn. If the CO2 level is extremely high (usually above 60 mm Hg) and the patient still has not attempted to take a single breath, the brainstem is unquestionably dead.
The Moment of Declaration
As soon as the apnea test is completed and positive, the patient is legally declared dead. The time of death recorded on the death certificate is not when the heart stops beating, but rather the exact time the apnea test was concluded.
At this point, life support is only maintained if the family agrees to organ donation. Otherwise, the ventilator is turned off, and the heart, deprived of oxygen, will stop beating within minutes.

Frequently Asked Questions (FAQ)
Why does the heart keep beating if the brain is dead?
The heart has its own internal electrical pacemaker (the sinoatrial node). It does not need the brain to tell it to beat. As long as the artificial lungs (the ventilator) keep supplying oxygen to the blood, the heart will continue to beat for days or even weeks after brain death.
Has anyone ever recovered from brain death?
No. By medical and legal definition, brain death is irreversible. Media stories about people who "woke up from brain death" are always cases where the person was in a deep coma but was never formally and correctly diagnosed with brain death using the rigorous protocols (like the apnea test).
Does the patient feel pain during the tests?
Absolutely not. The perception of pain occurs in the cerebral cortex. Because the entire brain has been destroyed, there is no capacity to feel pain, discomfort, or awareness of any kind.
Conclusion
Diagnosing brain death is one of the heaviest responsibilities an emergency or ICU physician carries. The process is designed to be infallible, eliminating any margin of doubt through rigorous clinical testing and the definitive apnea test.
For families, it is a brutal concept to accept due to the illusion of life provided by the machines. However, it is this exact artificial support that frequently allows for the miracle of organ donation, transforming a tragic loss into the salvation of multiple other lives.
This content is for educational and informational purposes only. It does not replace professional medical advice, diagnosis, or treatment. In case of a medical emergency, call 911/EMS immediately or go to the nearest emergency room.
References: [1] American Academy of Neurology (AAN): Evidence-based guideline update: Determining brain death in adults [2] StatPearls: Brain Death [3] UpToDate: Diagnosis of brain death [4] OrganDonor.gov: Brain Death